Every healthcare reimbursement begins the same way: a service is delivered to a patient and the provider submits a claim to the patient’s insurance company.
What happens next is a complex process known as the healthcare claim lifecycle. This lifecycle includes verification, authorization, claim submission, payer adjudication, and follow-up.
For revenue cycle teams, understanding how a claim moves through this process is essential. Small breakdowns at any stage can lead to delayed reimbursement or claim denial.
This article walks through the step-by-step lifecycle of a healthcare claim, from patient scheduling to final payment.
What Is the Healthcare Claim Lifecycle?
The healthcare claim lifecycle is the series of steps that occur between delivering medical services and receiving payment from an insurance company.
The process includes verifying insurance coverage, submitting claims to the payer, reviewing those claims, and resolving any issues before reimbursement is issued.
Although workflows vary across organizations, most healthcare claims move through the same core stages.
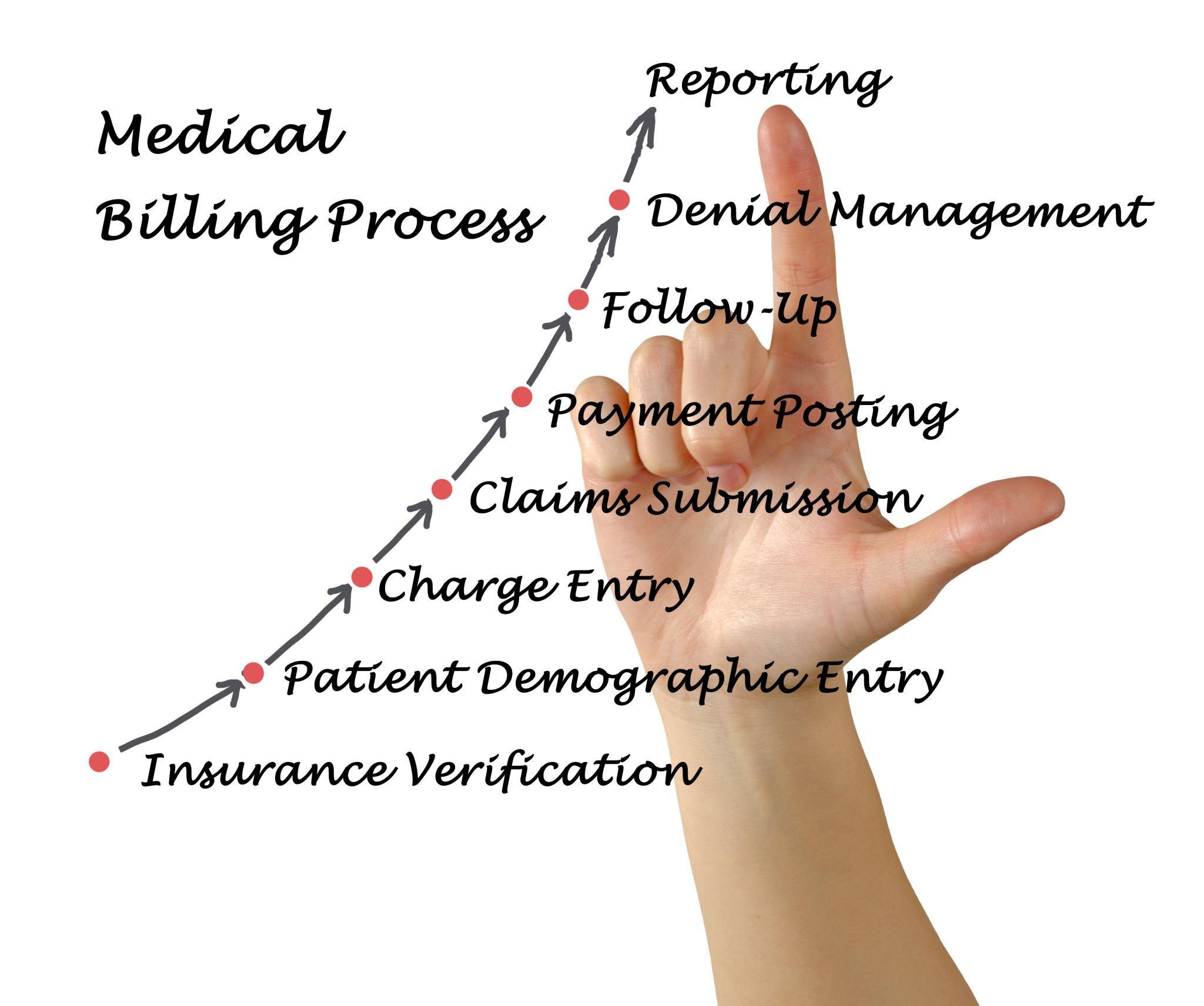
Key Takeaways
• The healthcare claim lifecycle includes all steps from patient insurance verification to final claim payment.
• Most claims pass through six core stages: eligibility verification, prior authorization, claim submission, payer adjudication, payment posting, and follow-up.
• Errors or missing information at any stage can delay reimbursement or lead to claim denial.
• Effective revenue cycle management focuses on preventing issues early and resolving payer delays quickly.
Step 1: Insurance Eligibility and Benefits Verification
The claim lifecycle begins before the patient arrives for care.
Revenue cycle staff verify that the patient’s insurance coverage is active and determine what services the plan covers.
During this step, staff typically confirm:
- policy status and effective dates
- deductible and out-of-pocket balances
- copay or coinsurance requirements
- coverage limitations
Many organizations perform this step through payer portals or direct insurance verification calls.
Accurate eligibility verification helps prevent billing errors and reduces the likelihood of claim denial later in the process.
Step 2: Prior Authorization (When Required)
Some services require insurance approval before treatment occurs. This process is known as prior authorization.
If authorization is required, providers must submit documentation explaining why the service is medically necessary.
Payers review this documentation and either approve or deny the request. Without authorization, the claim may later be rejected even if the treatment itself is covered.
Authorization requirements are especially common for:
- imaging services
- specialty medications
- surgical procedures
- high-cost treatments
Obtaining approval at this stage helps prevent delays in reimbursement.
Step 3: Charge Capture and Claim Creation
After the patient receives care, clinical documentation is translated into billable charges.
Medical coders assign standardized codes that describe the services provided.
These typically include:
- CPT codes describing procedures
- ICD-10 codes describing diagnoses
- HCPCS codes for supplies or additional services
This coded information is used to create the healthcare claim that will be submitted to the payer.
Accuracy at this stage is critical because coding errors are a common source of claim rejection.
Step 4: Claim Submission to the Payer
Once the claim is created, it is transmitted electronically to the patient’s insurance company through a clearinghouse.
The clearinghouse performs initial checks to confirm that the claim meets formatting and data requirements.
If the claim passes these checks, it is forwarded to the payer for review.
If errors are detected, the claim may be returned to the provider for correction before it ever reaches the insurance company.
Step 5: Claim Adjudication
After the payer receives the claim, it enters the adjudication process.
During adjudication, the insurance company reviews the claim to determine:
- whether the service is covered
- whether prior authorization was obtained
- whether coding is accurate
- how much reimbursement should be issued
The payer may:
- approve the claim and issue payment
- partially approve the claim
- deny the claim
- request additional documentation
Adjudication timelines vary depending on payer policies and claim complexity.
Step 6: Payment and Explanation of Benefits (EOB)
If the claim is approved, the insurance company issues payment to the provider.
At the same time, the payer sends an Explanation of Benefits (EOB) to both the provider and the patient.
The EOB outlines:
- total charges
- payer reimbursement amount
- patient responsibility
- adjustments or contractual discounts
Revenue cycle teams post this payment information to the patient account.
Step 7: Claim Follow-Up and Appeals
Not all claims are paid immediately.
Claims may remain pending, be denied, or require additional documentation. When this occurs, revenue cycle staff must follow up with the payer.
Common follow-up activities include:
- checking claim status through payer portals
- contacting insurance representatives
- submitting corrected claims
- appealing denied claims
Follow-up work often represents one of the most time-consuming parts of the claim lifecycle.
Because many issues require direct communication with insurers, payer phone calls remain a common part of the process.
Automation platforms such as SuperDial are increasingly used to manage these high-volume payer interactions while revenue cycle teams focus on resolving complex claim issues.
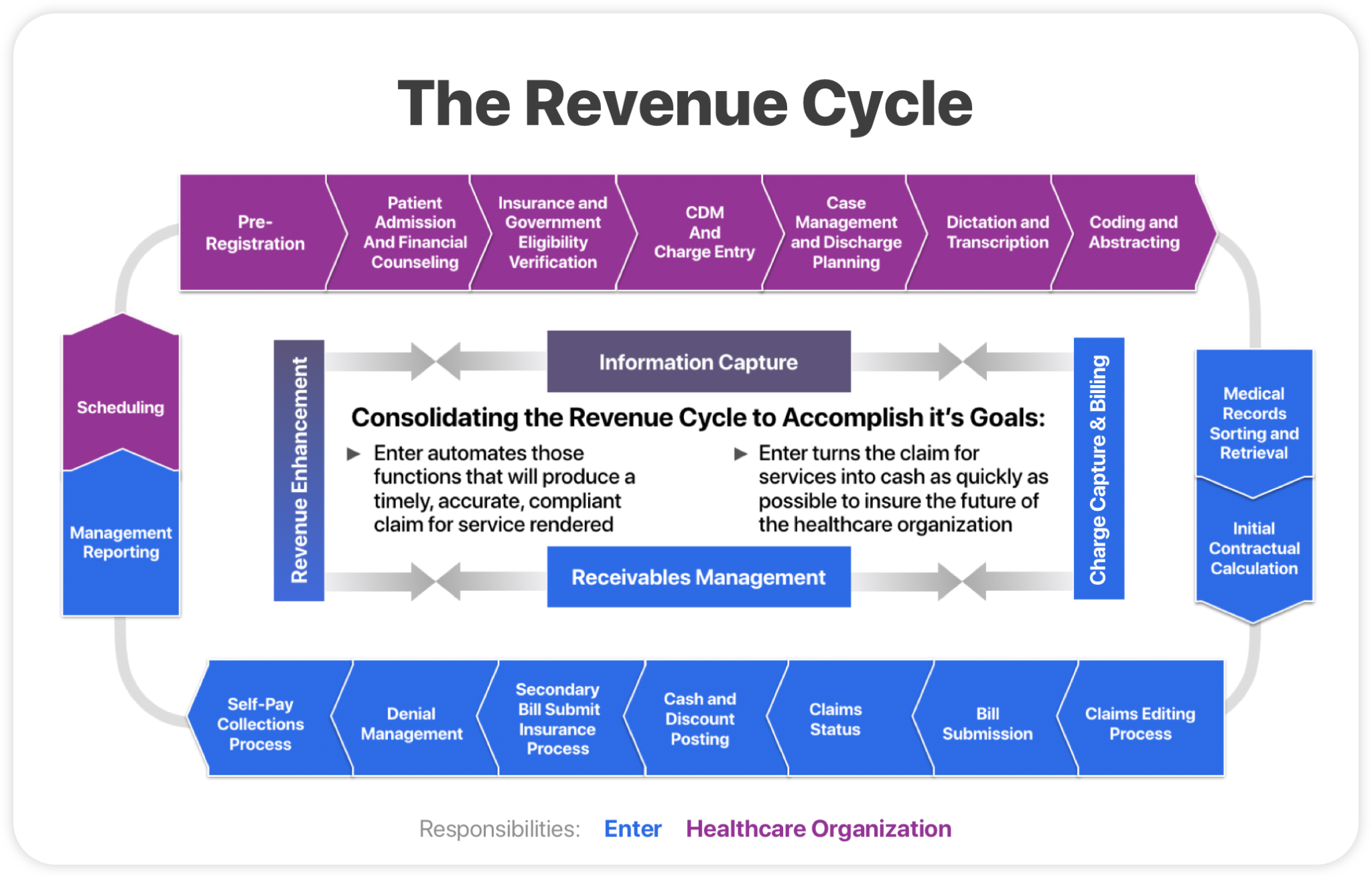
Why the Healthcare Claim Lifecycle Matters
The healthcare claim lifecycle determines whether providers are paid accurately and on time.
When each stage of the process runs smoothly, claims move quickly from service delivery to reimbursement. When breakdowns occur, payment delays and administrative workload increase.
For this reason, healthcare organizations invest heavily in revenue cycle management systems, workflow optimization, and payer communication strategies.
Understanding how claims move through the lifecycle helps organizations identify where delays occur and how to improve reimbursement performance.
Frequently Asked Questions
What is the healthcare claim lifecycle?
The healthcare claim lifecycle refers to the full process that occurs between delivering medical services and receiving payment from an insurance company. It includes eligibility verification, claim submission, payer adjudication, payment posting, and follow-up.
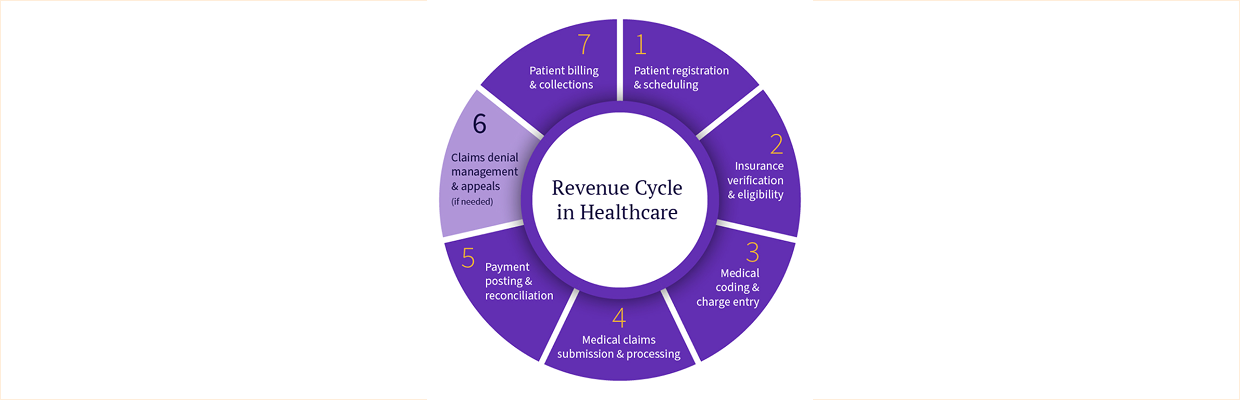
What are the main stages of the healthcare claim lifecycle?
Most healthcare claims pass through six core stages: eligibility verification, prior authorization (if required), charge capture and coding, claim submission, payer adjudication, and payment or follow-up.
Why do healthcare claims get delayed?
Claims are often delayed due to coding errors, missing documentation, authorization issues, or payer review processes. These issues may require follow-up or appeals before payment can be issued.
What role does revenue cycle management play in the claim lifecycle?
Revenue cycle management oversees the entire claim lifecycle. RCM teams verify insurance coverage, submit claims, track reimbursement, and resolve issues that prevent timely payment.
Final Perspective
The lifecycle of a healthcare claim may appear straightforward on paper, but in practice it involves dozens of operational steps across clinical, administrative, and payer systems.
Each stage — from eligibility verification to claim follow-up — plays a role in determining whether providers receive accurate and timely reimbursement.
For healthcare organizations, managing this lifecycle effectively is essential to maintaining financial stability and minimizing administrative burden.
.png)


.svg)