As dental service organizations scale, they solve one set of problems only to expose another. Centralized billing teams, standardized workflows, and shared systems make it possible to support dozens—or hundreds—of practices under a single operational umbrella. But that same scale can quietly overwhelm one of the most fragile parts of dental revenue cycle management: insurance phone calls.
For many dental service organizations, insurance-related calls have become a structural bottleneck rather than a temporary staffing issue. Eligibility checks, benefits verification, prior authorization follow-ups, and claims status calls all multiply as practices are added. What works for a single office quickly breaks at DSO scale.
To understand why this happens—and why AI is increasingly part of the solution—it helps to look at how insurance phone work is conducted inside a modern dental service organization.
Why insurance phone work breaks at DSO scale
Insurance phone calls are deceptively simple. A staff member calls a payor, waits on hold, navigates a phone tree, asks a few questions, documents the response, and moves on. In a single practice, this work is inconvenient but manageable.
In a dental service organization supporting dozens of locations, the math changes. Each practice generates eligibility questions, claim follow-ups, and authorization checks every day. Centralization consolidates this work into shared teams, but it doesn’t reduce the underlying volume—or the variability across payors.
Hold times vary. Phone trees change. Policies differ by plan, state, and procedure. Even experienced staff spend large portions of their day waiting, listening, or repeating the same conversations. As DSOs grow, insurance phone work becomes one of the least scalable components of the operation.
This is a natural consequence of the DSO model itself. As explained in What Is a Dental Service Organization (DSO)?, DSOs exist to centralize non-clinical functions. Insurance operations benefit from that centralization—but only up to the point where human labor becomes the limiting factor.
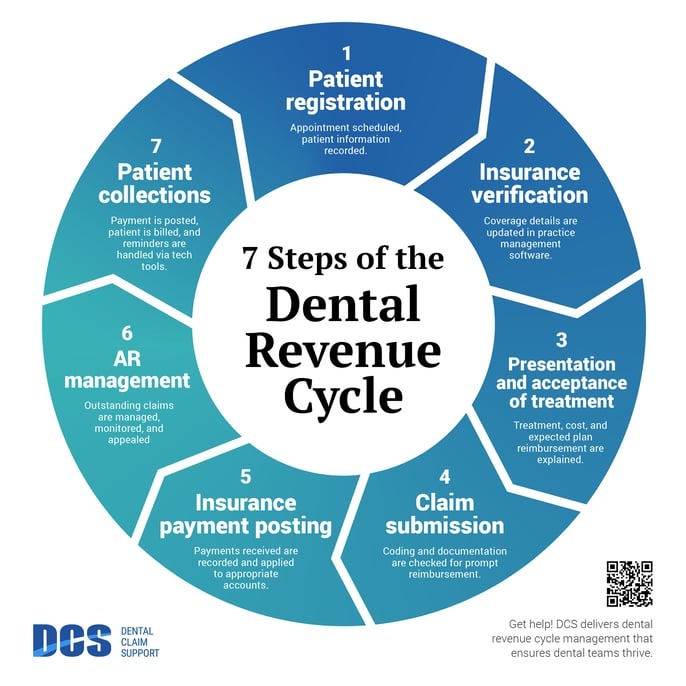
The hidden cost of manual insurance calls
The cost of insurance phone calls is often underestimated because it doesn’t appear as a single line item. It shows up instead as delayed payments, underutilized staff time, and avoidable write-offs.
When teams are stuck on hold, eligibility checks are delayed. When follow-ups slip, claims age unnecessarily. When staff are overwhelmed, documentation quality suffers. Over time, these small inefficiencies compound into measurable revenue leakage.
For DSOs backed by private equity or operating on thin margins, this drag is particularly painful. Scaling locations without addressing insurance phone workflows often means scaling headcount just to keep up—eroding the operational leverage that DSOs are meant to create in the first place.
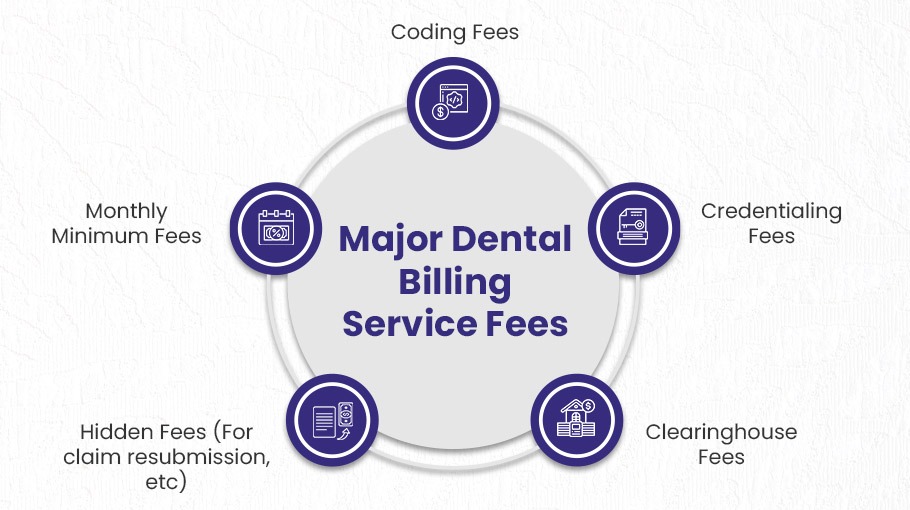
Why staffing alone doesn’t solve the problem
The most common response to insurance call overload is to hire more people. In the short term, this can help. In the long term, it rarely fixes the underlying issue.
Insurance phone work is highly repetitive, rules-driven, and dependent on external systems DSOs don’t control. Adding staff increases throughput linearly, but it doesn’t improve efficiency. Worse, turnover in these roles is high, which creates training churn and institutional knowledge loss.
Many DSOs eventually reach a point where insurance operations become a permanent bottleneck rather than a growing pain. At that stage, solving the problem requires a change in approach—not just more hands on the phones.
How AI changes the insurance phone equation
AI-driven phone automation introduces a fundamentally different model for handling insurance calls. Instead of relying exclusively on human staff to place and manage every call, DSOs can deploy AI agents to handle high-volume, repetitive interactions.
These systems are designed to navigate phone trees, wait on hold, ask structured questions, and capture responses automatically. Rather than replacing staff entirely, they absorb the most time-consuming parts of the workflow—freeing human teams to focus on exceptions, complex cases, and oversight.
For DSOs, this shift is particularly powerful because insurance workflows are highly standardized across practices. Eligibility checks and claim status calls follow predictable patterns, even when payor policies vary. That predictability makes them well-suited for automation at scale.
Where DSOs are seeing the biggest impact
DSOs adopting AI for insurance phone work tend to see the fastest results in a few specific areas.
Eligibility and benefits verification is often the first target. These calls are frequent, repetitive, and time-sensitive, making them ideal for automation. Prior authorization follow-ups are another high-impact area, especially when authorizations stall due to missing information or slow responses.
Claims status calls also benefit from automation, particularly for aged claims that require repeated follow-up. Rather than tying up staff with dozens of similar calls, AI systems can manage the volume and escalate only when human intervention is required.
The common thread across these use cases is leverage. AI allows DSOs to handle more insurance interactions without proportionally increasing headcount.
AI as an extension of the DSO operating model
Importantly, AI-driven insurance automation aligns closely with the original logic of the dental service organization model. DSOs exist to centralize, standardize, and professionalize non-clinical operations. AI extends that logic by removing human wait time and repetition from the equation entirely.
Rather than forcing DSOs to choose between scale and control, AI makes it possible to grow without compounding administrative friction. Insurance phone calls stop being a growth constraint and become a managed system.
This doesn’t eliminate the need for experienced revenue cycle staff. It changes how their time is spent. Humans move up the value chain, focusing on judgment, escalation, and optimization rather than endurance.
What this signals about the future of DSO operations
Insurance phone bottlenecks are not a temporary artifact of growth—they are a structural challenge inherent in payor-driven healthcare systems. DSOs that treat them as such are increasingly looking beyond staffing models and toward automation.
As AI becomes more capable and more integrated into revenue cycle workflows, DSOs that adopt early are likely to see compounding advantages: faster cash flow, lower administrative costs, and more resilient operations.
In that context, AI-driven insurance phone automation isn’t a bolt-on tool. It’s a natural evolution of how dental service organizations fulfill their core promise—allowing clinicians to focus on care while the business runs at scale.
For DSOs evaluating their next phase of growth, the question is no longer whether insurance phone work can be optimized, but whether it still makes sense to manage it manually at all.
.png)



.svg)